For a decade, the promise of artificial intelligence in medicine has been measured in press releases and venture capital rounds. The pitch never changed: AI would compress drug discovery timelines from fifteen years to three, slash billion-dollar development budgets, and reverse the pharmaceutical industry's notoriously stubborn 90 percent clinical failure rate.
In 2026, that pitch is finally being tested against actual patient data.
A handful of drugs designed entirely by AI are now inside human bodies. Not optimized or screened using AI as a supporting tool, but conceived and built by AI from the ground up. Some are in mid-stage trials. At least one has produced peer-reviewed clinical evidence of efficacy. Over the next twelve months, pivotal Phase III readouts will either validate a decade of ambition or force the industry to reckon seriously with what AI can and cannot do in medicine.
The Milestone That Changed the Conversation
The drug at the center of this story is rentosertib, developed by Insilico Medicine and formerly known as ISM001-055. It holds a specific distinction in the history of medicine: it is the first drug in which both the disease target and the molecular compound were discovered using generative AI, making it what the industry now calls a fully end-to-end AI-designed therapeutic.
The disease it targets is idiopathic pulmonary fibrosis (IPF), a progressive and largely incurable lung condition that kills most patients within two to five years of diagnosis. Existing approved therapies can slow disease progression, but none reverse it.
Insilico's generative AI platform, called Pharma.AI, was pointed at this problem in 2019. It identified a novel disease target called TNIK, a protein kinase that drives fibrosis pathways, then designed a small molecule to inhibit it. The entire preclinical development program, from hypothesis and target discovery through to drug candidate generation, took just under 18 months to complete at a budget of around $2.6 million.
By the standards of pharmaceutical R&D, where a single compound can take years and tens of millions of dollars to reach preclinical candidacy, that timeline was remarkable. What followed was not so different: the drug still had to navigate the same Phase 0, Phase I, and Phase II clinical trials that any candidate must clear. There are no AI shortcuts in clinical testing.
The Phase IIa Results
In November 2024, Insilico announced positive topline results from the Phase IIa trial. The study was a randomized, double-blind, placebo-controlled trial enrolling 71 patients with IPF across 21 sites in China.
At the highest dose of 60 mg once daily, patients showed a mean improvement of 98.4 mL in forced vital capacity (FVC) from baseline. The placebo group, by contrast, showed a mean decline of 62.3 mL. The drug was well-tolerated across all dosing groups.
In June 2025, Insilico published the industry's first proof-of-concept clinical validation of AI-driven drug discovery in Nature Medicine. The company is now in discussions with regulatory authorities about a Phase IIb pivotal trial, while a separate Phase IIa trial in U.S. patients is actively enrolling.
That published result is the most significant milestone this field has produced. It is also, as most researchers are careful to note, a starting point rather than a finish line.
A Pipeline That Is No Longer Hypothetical
Rentosertib is the furthest along, but it is far from alone. The AI drug pipeline has grown from a handful of early-stage curiosities into a substantial clinical portfolio.
As of early 2026, over 173 AI-discovered drug programs are in clinical development, with 15 to 20 expected to enter pivotal trials during the year.
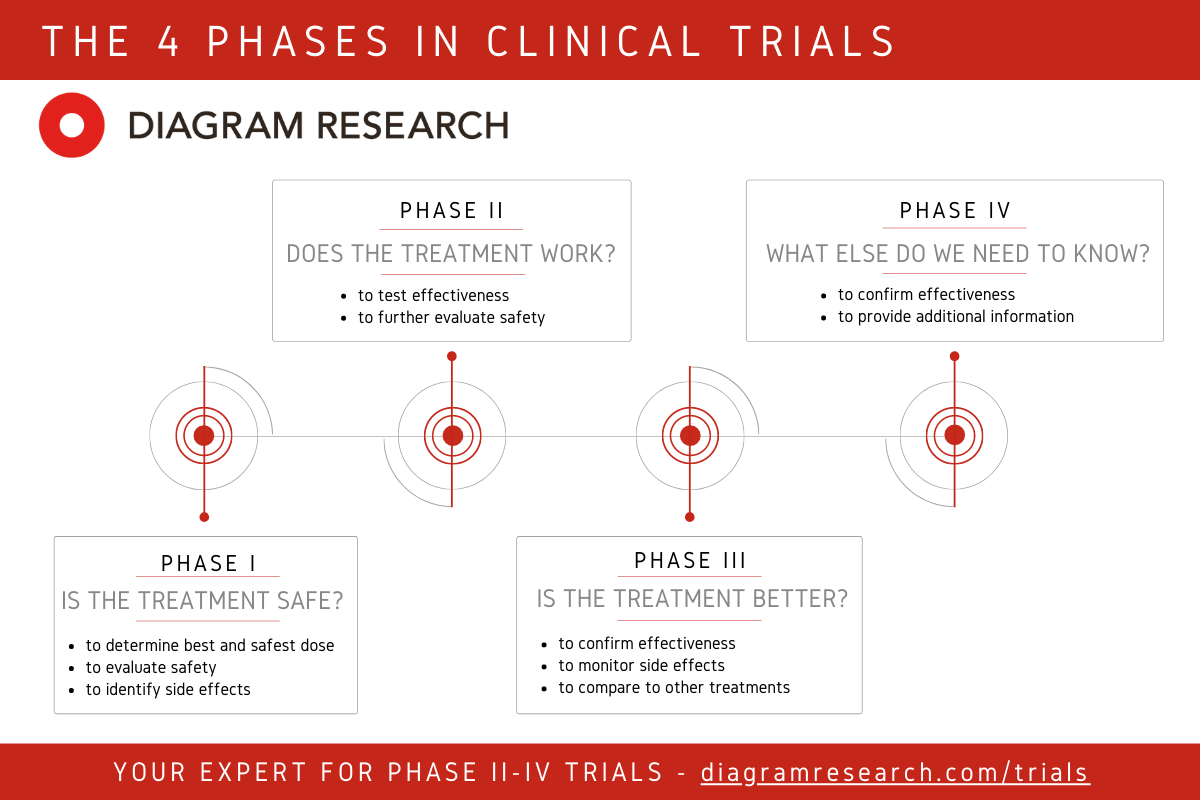
The current pipeline breakdown:
- Phase I: approximately 94 programs
- Phase II: approximately 56 programs
- Phase III: approximately 15 programs
That Phase III number is the one the industry is watching most closely.
Recursion and Exscientia
The two companies completed their merger in mid-2025, combining Recursion's high-throughput biological imaging capabilities with Exscientia's precision molecular design tools into a single end-to-end platform. The merged entity now has more than 10 clinical and preclinical programs in its internal pipeline and over $20 billion in potential milestone payments from partners.
Key 2026 pipeline updates include a Phase 2 readout for REC-394 in C. difficile infection and Phase 1 data for REC-1245, an RBM39 degrader in oncology.
Schrödinger and Takeda
Schrödinger uses a physics-based AI approach rather than purely data-driven generative models. Its compound zasocitinib, developed through a partnership with Nimbus Therapeutics and later acquired by Takeda, is now in Phase III.
Takeda reported in December 2025 that the AI-designed molecule eased the severity of plaque psoriasis in two late-stage trials. That result positions zasocitinib as a leading candidate for what may become the first FDA approval of an AI-discovered drug.
Isomorphic Labs
The Google DeepMind spinout has not yet advanced compounds into clinical trials, but its technological position is formidable. In January 2026, Isomorphic Labs announced a research collaboration with Johnson and Johnson, leveraging its IsoDDE drug design engine for multi-modality drug discovery across small molecules and biologics.
The company's platform reportedly more than doubles AlphaFold 3's accuracy on challenging protein-ligand structure prediction benchmarks, which matters directly for identifying viable drug targets and predicting how tightly a molecule will bind.
What the Early Success Rates Actually Show
The emerging clinical data on AI-discovered drugs deserves careful interpretation rather than uncritical celebration or easy dismissal.
Phase I performance is striking. AI-discovered molecules are achieving success rates of 80 to 90 percent in early human trials, significantly higher than the roughly 52 percent historical average for traditional methods. This reflects something real: AI platforms are substantially better at predicting which compounds will be safe and well-tolerated before they ever reach clinical testing. Better early filtering means fewer surprises when humans are first dosed.
Phase II performance is encouraging but still limited by sample size. AI-discovered drugs are showing approximately 65 to 75 percent success rates compared to 30 to 45 percent for traditional approaches.
Phase III is where the real test lies. The pharmaceutical industry's persistent overall failure rate is driven heavily by late-stage failures, where drugs that worked in smaller trials turn out not to work in larger and more diverse patient populations. AI has not yet demonstrated that it can materially change those odds.
The honest framing: AI has made the early part of drug development faster and cheaper. Whether it can make the clinical part more successful is the question 2026 is beginning to answer.
The Setbacks Worth Acknowledging
In May 2025, Recursion discontinued its lead AI-discovered candidate REC-994 for cerebral cavernous malformation after long-term data did not confirm earlier efficacy trends. Earlier, in 2023, AI-designed compounds missed endpoints in trials for atopic dermatitis, schizophrenia, and cancer.
These failures are a useful corrective to any narrative that treats AI drug discovery as a guaranteed improvement on traditional methods. Failure rates in clinical medicine are stubborn, and AI has not yet proven it can tame them.
How the Technology Actually Works
The term "AI drug discovery" covers a range of meaningfully different technical approaches, and the distinctions matter for understanding what each platform can and cannot do.
Generative Chemistry
This is the approach Insilico Medicine uses, and the most widely discussed in public coverage. Generative AI learns the relationship between molecular structure and biological activity across millions of known compounds, then designs new candidates optimized for potency, selectivity, and favorable pharmacokinetic properties.
During the rentosertib program, Insilico's Chemistry42 platform generated 78,000 virtual TNIK inhibitors, filtered these through multi-objective optimization, and synthesized the 60 top-ranked compounds. The hit rate was 16.7 percent. Traditional high-throughput screening typically produces hit rates around 0.1 percent.
Physics-Based AI Design
Schrödinger's approach combines quantum mechanical simulations with machine learning to predict how molecules interact with protein targets at the atomic level. This is computationally intensive, but it makes highly accurate binding predictions for targets where structural data is available.
It's better understood as AI-enhanced physics rather than purely data-driven generation, and it is particularly well-suited to targets where three-dimensional binding geometry is critical to efficacy.
Phenomics and Biological Imaging
Recursion's platform images cells under thousands of different conditions and uses computer vision to detect biological patterns that human researchers would miss. This approach excels at target identification, surfacing which biological pathways are relevant to a disease and feeding higher-quality hypotheses into downstream chemistry work.
Structural Biology AI
AlphaFold's protein structure predictions have become foundational across the industry. By 2026, scientists working on complex biologic modalities are routinely evaluating binding affinity computationally before committing resources to experimental validation.
Isomorphic Labs' IsoDDE builds on AlphaFold with improvements specifically targeted at drug-receptor binding prediction, the step most directly relevant to whether a designed molecule will actually work.
Most advanced platforms combine several of these approaches across different stages of the discovery pipeline, deploying each tool where it has the strongest advantage.
Big Pharma's Shift from Skepticism to Infrastructure
The major pharmaceutical companies are no longer watching the AI drug discovery space from a cautious distance. The question now is not whether to integrate AI into R&D, but how to do it at scale with enough governance to satisfy regulators.
Novartis has built a proprietary data lake called Data42, containing over 30 years of clinical and preclinical studies. The company uses AI to generate activity profiles for heart muscle cells to predict potential cardiac toxicity before compounds advance to clinical testing. Novartis' head of biomedical research has been publicly clear-eyed about the limits: AI can replace some bench-level science, but not all.
AstraZeneca has reported more than 50 percent faster target drug design and validation in early discovery programs where it has applied AI. That kind of concrete operational improvement drives adoption decisions regardless of what eventually happens in Phase III trials.
Pfizer plans to spend $11 billion on R&D in 2026 and is pairing AI engineers with scientists across the organization to measure productivity systematically. The integration is less about replacing scientists and more about compressing the design-make-test-analyze cycle that defines modern medicinal chemistry.
The Regulatory Picture Is Finally Taking Shape
One factor that has slowed commercial development of AI drug discovery is regulatory uncertainty. Drug regulators needed to develop frameworks for evaluating AI-generated evidence before companies could build compliance infrastructure around it.
The FDA issued its first draft guidance on the use of AI in supporting drug regulatory decisions in January 2025. This was followed in January 2026 by joint guiding principles published by the FDA and the European Medicines Agency on good AI practice in drug development.
Key regulatory milestones to watch in 2026:
- Q2 2026: FDA finalizes AI guidance, requiring credibility assessment plans for high-risk applications and detailed documentation on model architectures, training data, and governance
- August 2, 2026: EU AI Act's high-risk provisions take effect, potentially classifying some drug development AI as high-risk with new compliance requirements
Documentation requirements under the FDA framework scale with risk level. Low-risk hypothesis-generating tools face minimal requirements. High-risk uses, such as analyzing clinical trial data or selecting trial participants, require full transparency, prospective validation, and ongoing monitoring.
The documentation burden is real, and some smaller companies will struggle to meet it. But a clear regulatory framework is ultimately better for the industry than the previous ambiguity. Companies can now build compliance infrastructure around known requirements.
The Honest Assessment: What AI Cannot Change
The most important thing to understand about AI drug discovery in 2026 is where the technology's limits genuinely lie.
Clinical timelines remain unchanged. Clinical trial duration, regulatory review timelines, and manufacturing scale-up are not meaningfully accelerated by AI. Biology, patient enrollment, and regulatory requirements impose constraints that algorithms cannot bypass. Claims of ten times faster drug development conflate preclinical acceleration with total development timelines, a misleading framing that the industry's own researchers have pushed back against.
AI delivers measurable value in early discovery. It does not fundamentally alter pharmaceutical development economics. The technology reduces one component of a multi-year process without changing the rate-limiting steps.
Training data biases are a serious unresolved problem. Training data for AI drug discovery systems is heavily skewed toward European genomics and common diseases, which means predictions are materially less accurate for underrepresented populations. If AI-discovered drugs systematically work better for some groups than others because of this, it creates both a scientific and an ethical problem the industry will need to address before AI drug discovery can claim to be broadly beneficial.
Market consolidation is already sorting the field. Smaller AI drug discovery companies face existential pressure as investors demand clinical results rather than algorithmic demonstrations. Expect acquisitions, shutdowns, and pipeline deprioritizations over the next 12 to 18 months as the market separates companies with genuine clinical validation from those that raised money on early promise alone.
What 2026 Will Actually Decide
The most consequential development of this year will not be a funding round or a partnership announcement. It will be Phase III readouts.
These results will provide the first large-scale test of whether AI improves clinical success rates beyond the industry's persistent 90 percent failure rate. If multiple AI-discovered compounds show efficacy where traditionally discovered drugs with similar profiles would have failed, that is a meaningful signal. If they fail at the same rate, it suggests that AI's contribution, while real and valuable in early discovery, does not fundamentally change the odds of clinical success.
A realistic forecast for 2026 is validation and disappointment in roughly equal measure. Positive Phase III data from one or two programs would be significant evidence for the field's core thesis. Some highly anticipated trials will also almost certainly fail, as they do in every pharmaceutical development cycle.
A first FDA approval remains plausible in 2026 or 2027, with roughly 60 percent probability according to analysts tracking the pipeline. That estimate reflects genuine uncertainty, not hedging.
Conclusion
The AI drug discovery story is no longer a future-tense narrative. Rentosertib is in patients. Zasocitinib has late-stage trial data. More than 170 AI-originated programs are in clinical testing. The field has crossed from promising technology into the early stages of clinical proof.
What it has not yet done is demonstrate that AI materially improves the odds of success in the trials that matter most. That evidence, or its absence, is what 2026 is positioned to deliver.
For patients with diseases like idiopathic pulmonary fibrosis who have limited treatment options, and for the pharmaceutical industry trying to justify a decade of AI investment, the stakes of those readouts are real. The machines have designed the drugs. Now biology gets a vote.
Frequently Asked Questions
What is the first fully AI-designed drug to reach clinical trials?
Rentosertib, developed by Insilico Medicine and formerly known as ISM001-055, is widely considered the first drug in which both the disease target and the molecular compound were identified and designed entirely using generative AI. It is currently in Phase IIa clinical trials for idiopathic pulmonary fibrosis, with positive results published in Nature Medicine in June 2025.
How many AI-discovered drugs are currently in clinical development?
As of early 2026, more than 173 AI-discovered drug programs are in some stage of clinical development. The breakdown is roughly 94 programs in Phase I, 56 in Phase II, and 15 in Phase III, with 15 to 20 programs expected to enter pivotal trials during 2026.
Do AI-discovered drugs have better clinical success rates than traditional drugs?
Early data suggests AI-discovered compounds achieve 80 to 90 percent success rates in Phase I, significantly higher than the roughly 52 percent historical average for traditional methods. Phase II rates also appear higher. However, Phase III results, where most pharmaceutical failures occur, remain limited. The 2026 pivotal readouts are the first large-scale test of whether AI's early advantage translates to better ultimate outcomes.
Which companies are leading in AI drug discovery in 2026?
The leading clinical-stage companies include Insilico Medicine, which has the most advanced fully end-to-end AI-designed compound; the combined Recursion-Exscientia entity; Schrödinger, whose compound zasocitinib has Phase III data through a Takeda partnership; and Relay Therapeutics. Isomorphic Labs, backed by Google DeepMind, has significant technological capabilities but has not yet advanced compounds into clinical trials.
Has the FDA approved any AI-discovered drugs?
No AI-discovered drug has yet received FDA approval as of early 2026. The first approval is estimated to have roughly a 60 percent probability of occurring in 2026 or 2027, depending on ongoing trial outcomes. Rentosertib and zasocitinib are the most advanced candidates.
What is the FDA doing to regulate AI in drug development?
The FDA issued its first comprehensive draft guidance on AI in drug development in January 2025. Final guidance is expected in Q2 2026, requiring credibility assessment plans for high-risk AI applications. In January 2026, the FDA and the European Medicines Agency jointly published guiding principles for good AI practice in drug development. The EU AI Act's high-risk provisions take effect in August 2026.
How does AI actually design drugs?
AI drug discovery uses several technical approaches. Generative chemistry platforms design novel molecular structures from scratch by learning from millions of known compounds. Physics-based AI combines quantum mechanical simulations with machine learning to predict molecular interactions. Biological imaging platforms use computer vision to identify disease-relevant cellular patterns. Structural biology AI predicts protein structures and binding interactions. Most advanced platforms combine several of these approaches across different pipeline stages.
Can AI eliminate the pharmaceutical industry's 90 percent clinical failure rate?
Probably not entirely, and certainly not soon. AI can compress early-stage discovery timelines and improve the quality of candidates entering trials, which may improve Phase I and II success rates. But clinical trials remain driven by biology and regulatory timelines that AI cannot accelerate. Whether AI changes Phase III success rates, where most failures occur, is the central question that 2026's data will begin to answer.
Related Articles